1) Welcome to an #accredited #tweetorial on a patient’s perspective of the clinical course of #ADPKD. Earn 0.5h CME/CE credit #physicians #nurses #nursepractitioners #physicianassistants #geneticists #hepatologists by following this 🧵. I am Tess Harris @Elektra of @PKDCharity 🇬🇧

2) This program is supported by an educational grant from Otsuka Pharmaceuticals & is intended for healthcare providers. Faculty disclosures http://www.ckd-ce.com/disclosures. Learn more about #ADPKD & earn MORE credit https://ckd-ce.com/adpkd1/. Follow us! @fjcaskey @NWiegley @pecoitsfilho
3) Medical disclaimer: I’m not a physician. This program is based on mix of 40+ yrs lived experience & 17 years representing #ADPKD patients worldwide. @PKDCharity @PKD_Int @ErkNet @Song
4) My framework is ‘ADPKD Route Map’ (2018) https://pkdinternational.org/downloads/adpkd-route-map/ADPKD_Patient_Route_Map_INTERNATIONAL_ENGLISH_2018_06_01.pdf. It was developed by #HCPs & patients to explain types of care & support patients and families should expect from a health service.
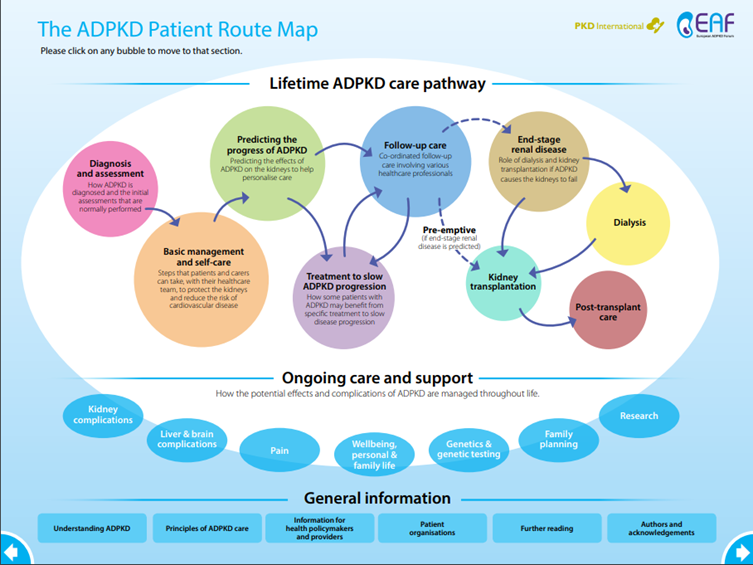
5) #ADPKD most common inherited kidney disease. 5% ESRD in ; 8-10% . Heterogenous inter/intrafamilial. Mainly caused by 2 genes PKD1 (78%) & PKD2 (15%). Newer rarer genes inc GANAB, DNAJB11, ALG9 & IFT140. 5-10% de novo diagnoses.
6) How is #ADPKD diagnosed?
a) tested/screened’ in childhood due to family history
b) during exam for other reason, eg #hypertension, suspected kidney stone, haematuria, pregnancy
c) incidentally, eg scan following abdominal injury/surgery.
7) The diagnosis is often a shock to patient/parent; many describe feeling ‘devastated’, others have ‘genetic guilt’ when told
8) Historically, ultrasound imaging was sufficient for diagnosis, using unified criteria (2009) for adults https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2615723/. Recently pts are offered CTs, MRIs & genetic testing. Other tests inc bloods, urine, BP.
9) Please respond by commenting: how do you diagnose #ADPKD in your patients? U/S, CT, MRI, exome sequencing (WES), whole-genome sequencing (WGS), other tests?
10) Initial treatments are symptomatic esp #BP (~7 in 10 at diagnosis); suggested target 110/75, than in #CKD. Chronic pain may be reported but limited treatments available. DIPAK Consortium proposed helpful stepwise approach for management
11) At specialist centres, pts might be referred for known non-kidney manifestations eg brain aneurysm scans, liver cyst evaluation, pain, family planning/genetic counselling. But this not usual. In early stage, eGFR is high/stable . . .
12) . . . & pts are generally little more & told to return in a year. This is when they turn to ‘Dr Internet’ for help & discover that #ADPKD is ‘more than a kidney disease. (refer again to https://pkdinternational.org/downloads/adpkd-route-map/ADPKD_Patient_Route_Map_INTERNATIONAL_ENGLISH_2018_06_01.pdf)
13) Personal note: I was diagnosed over the phone after family screening. Pre-internet era, went to medical bookshop, discovered #ADPKD was incurable & average age of death was 57. My father died at 57 ironically.
14) My enlightened kidney doctor gave me annual creatinine results, which I graphed from 1983. Alas, I showed a classic PKD1 trajectory, #PD in 2019, DCD #Txp 2020 (at later age than siblings due to heterogeneity).
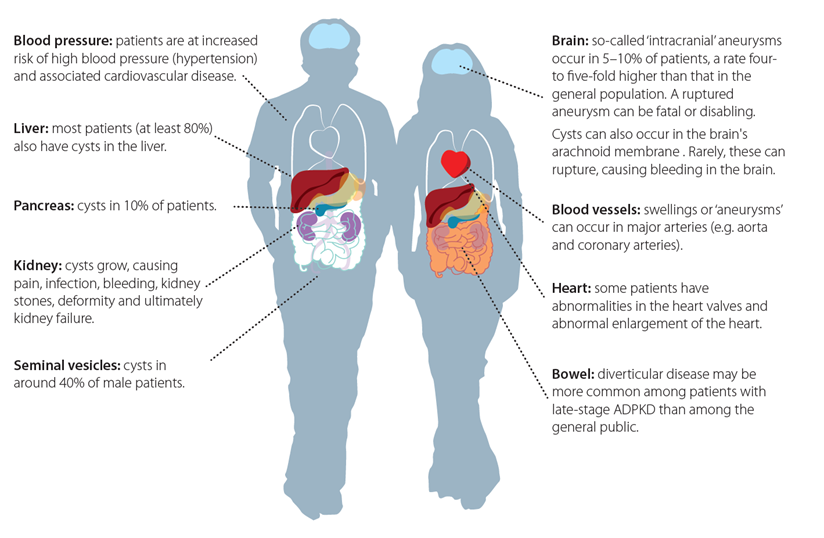
15) Non-kidney (‘extra-renal’) manifestations don’t always manifest, but many do at diagnosis or over time. 8-10% have brain aneurysms (twice general population), which occasionally lead to postmortem diagnosis.
16) Bursting rarely but devastatingly, pts understandably fear them. Aneurysms were ranked 5th most important outcome in #SONG-PKD
17a) Liver cysts for many pts have been the most surprising. Historically, pts never knew unless told incidentally by radiographer or at pre-transplant scan. 8-9 in 10 adults have cystic livers.
17b) If >20 cysts, this is #PLD (polycystic liver disease) of which 5% have massive hepatomegaly (enlarged liver), with surgical implications.
18) However, many will experience pain from hepatomegaly (plus cystic kidneys) & cyst infections. Resulting abdominal distention can cause body dysmorphia. “When are you due?” is common. [Images shown with permission]
19) Check your knowledge: All #ADPKD patients will have #PLD?
20) Mark your response and RETURN TOMORROW for more education and for a link to your🆓 CE/#CME! 👏to @sibgokcay @DiMiRenalMD @rajmehrotra1122 @silvishah @DrMattGB @CharlieTomson @AmandaPichini @kamkalantar @RClaure_nefro @BaanCarla @drmanishasahay @HPB_Txp_Surg @stephenmcadoo
21) Welcome back! We're discussing the patient perspective on #ADPKD and YOU are earning 🆓CE/#CME 🇬🇧🇪🇺🇨🇦🇺🇸! I am @Elektra. Thanks for joining us–now FOLLOW us!
@whatsthegfr @PkdResearch @KattyParker84 @PeterPReese1 @DrKidneyAsh @drpriyajohn @elliotktannor @anitavanzwieten
22) Yesterdays poll? It's FALSE, but not by much. Per 🔓https://www.ncbi.nlm.nih.gov/books/NBK373392/, patients with #ADPKD have associated #PLD in 75% -90% of cases.

23) Other issues faced by the typical pt w/ ADPKD include infections (UTIs, kidney/liver cysts), #kidneystones, benign cysts (brain, pancreas, throat), bowel #diverticula, heart (mitral valve prolapse, #LVH). See 🔓
24) As in any #CKD, #ADPKD pts experience other ‘unpleasant symptoms’ with kidney function decline 🔓
25) Due to genetic & other factors, progression of #ADPKD is difficult to predict. Can consider biomarkers, #eGFR, Total Kidney Volume (#TKV) or 🧬 mutation, ♂️/♀️, age at #hypertension onset, or 1st urological sign.
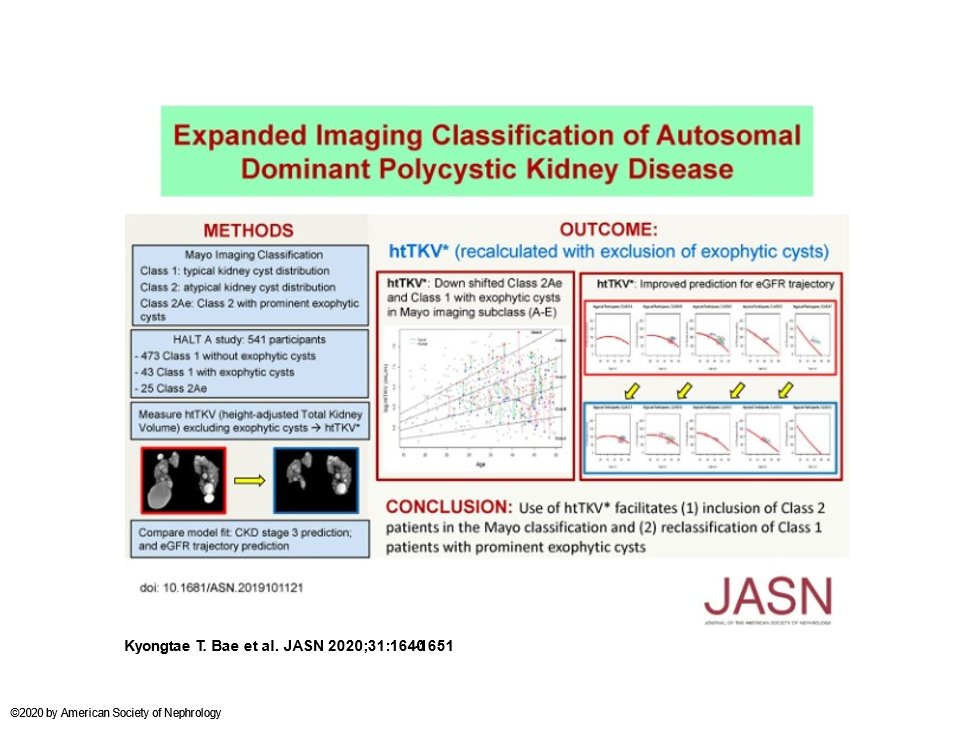
26) There are #ADPKD prediction scores, including #PROPKD (🔓https://www.ncbi.nlm.nih.gov/labs/pmc/articles/PMC4769200/) & Mayo Classification (below,🔓https://jasn.asnjournals.org/content/31/7/1640).
27) To date, only 1⃣ disease-modifying #ADPKD treatment, #tolvaptan, has been authorised: 2015 in 🇪🇺https://www.ema.europa.eu/en/medicines/human/EPAR/jinarc & 2018 in 🇺🇸https://www.accessdata.fda.gov/drugsatfda_docs/nda/2018/204441Orig1s000TOC.cfm.
28) Treatment algorithms vary: 🇺🇸🔓 https://jasn.asnjournals.org/content/29/10/2458, and 🇪🇺🔓
29) Please respond by commenting: how do you decide whom to treat with tolvaptan? Mayo Classification, PROPKD, eGFR decline rate, genetic mutation, family history, other?
30) For those who reach end stage kidney disease (ESKD), kidney replacement therapy (KRT) is only option to survive. Typical ESKD < 60 yrs in 🇪🇺. See 🔓
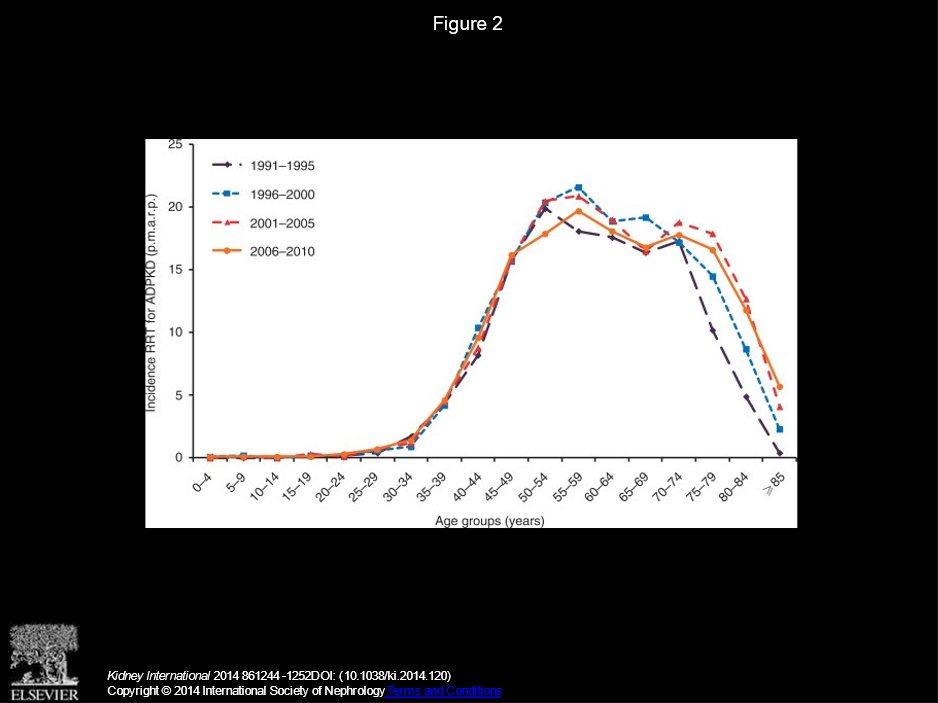
31) #KRT choices: Living/deceased donor transplant, peritoneal dialysis, haemodialysis. Sometimes, pre or post-transplant #ADPKD pts have kidneys removed (nephrectomies) due to size, pain, infections.
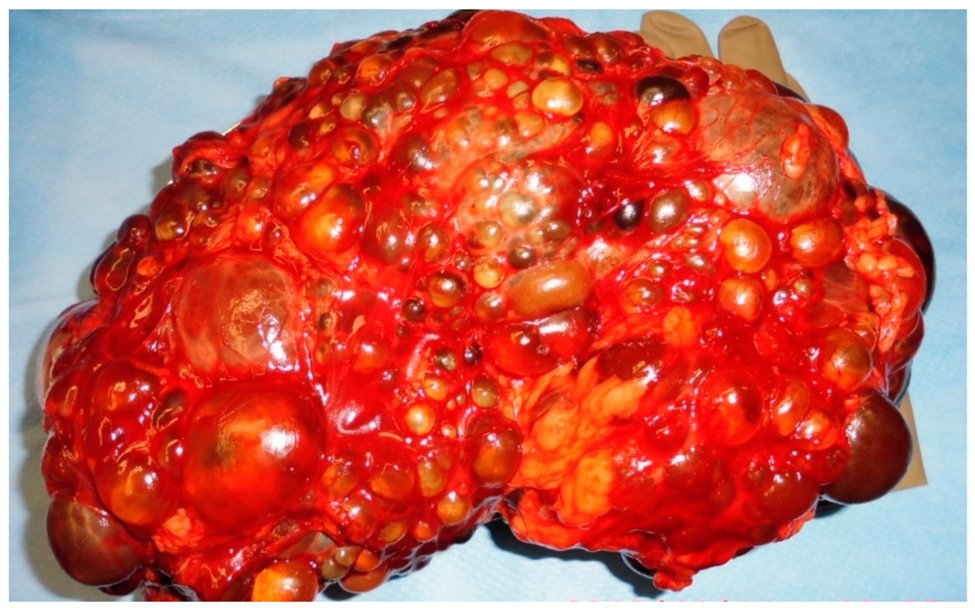
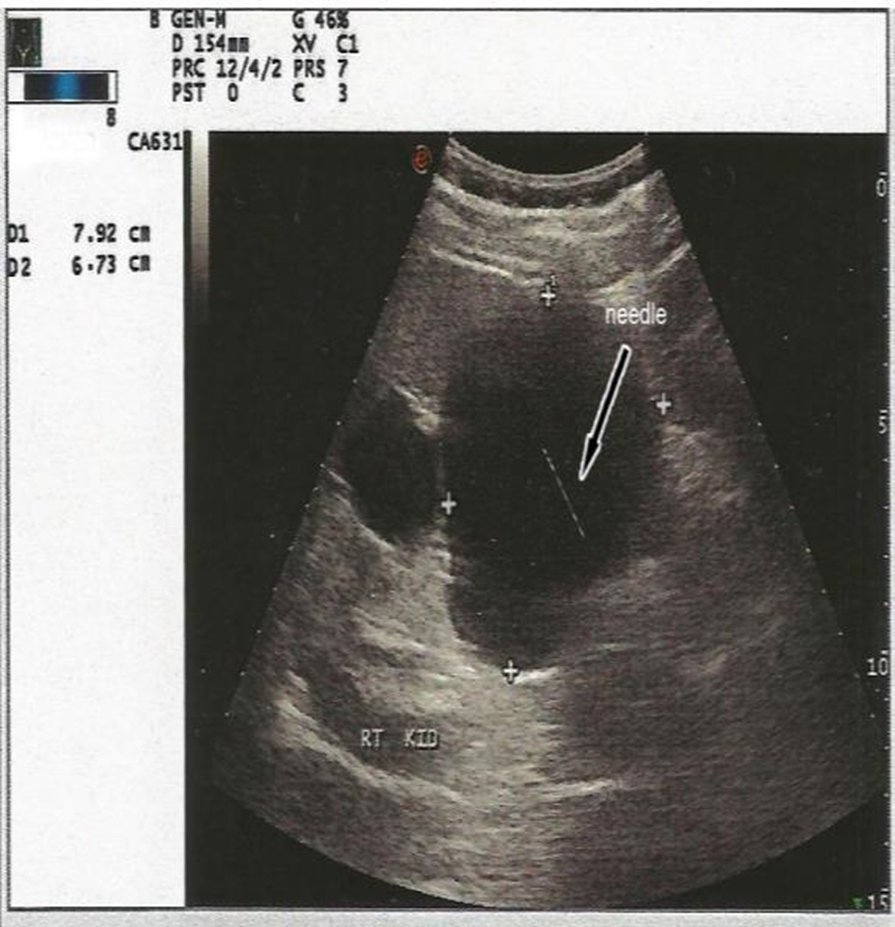
32) Other surgical interventions in #ADPKD inc kidney cyst aspiration/deroofing (fenestration), aneurysm coiling, hernia fixing, liver resection or transplantation.
33) Psychosocial & economic burden #ADPKD patients’ & caregivers/family #QOL, #anxiety, #depression, ability to work & life participation. Care ‘outside clinic’ @PKDFoundation @PKDCharity @PKD_eV @endPKD @AIRPonlus @PKD_Australia
34) Don’t forget the children! #ADPKD was considered ‘adult’ condition but they do present with symptoms, especially ⬆️ #BP. 🔓
35) #ADPKD guidelines? Awaiting @goKDIGO Guidelines ‘24/25. ITM: 🔓https://linkinghub.elsevier.com/retrieve/pii/S2157171615321468. For children/young people: 🔓
36) 🔬Hope on the horizon. But #ADPKD is complex! Research continues into cyst formation/growth, progression biomarkers, genetic modifiers, #cilia role, cytoskeleton. Nice summary of tools 🔓https://www.ncbi.nlm.nih.gov/labs/pmc/articles/PMC7352572/ :
37) Translational #ADPKD research into new molecules & repurposed meds, dietary interventions targeting different pathways. Selection of studies/trials: 🔓https://clinicaltrials.gov/ct2/results?cond=adpkd&Search=Apply&recrs=b&recrs=a&recrs=f&recrs=d&age_v=&gndr=&type=Intr&rslt=
And there is no shortage of targets, as per 🔓https://www.kidney-international.org/article/S0085-2538(15)53934-3/fulltext#relatedArticles:
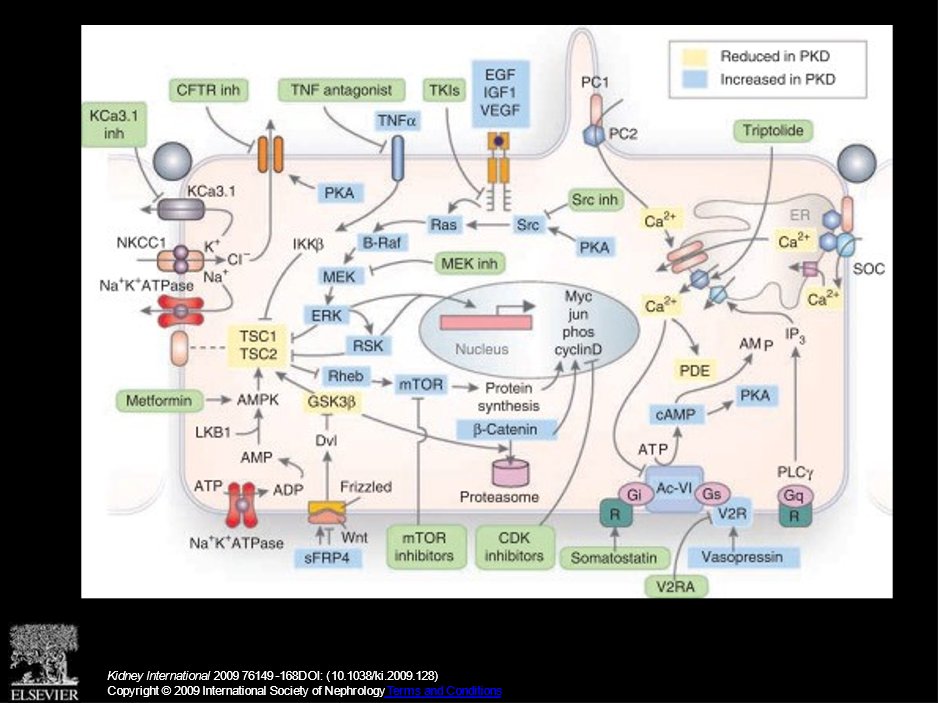
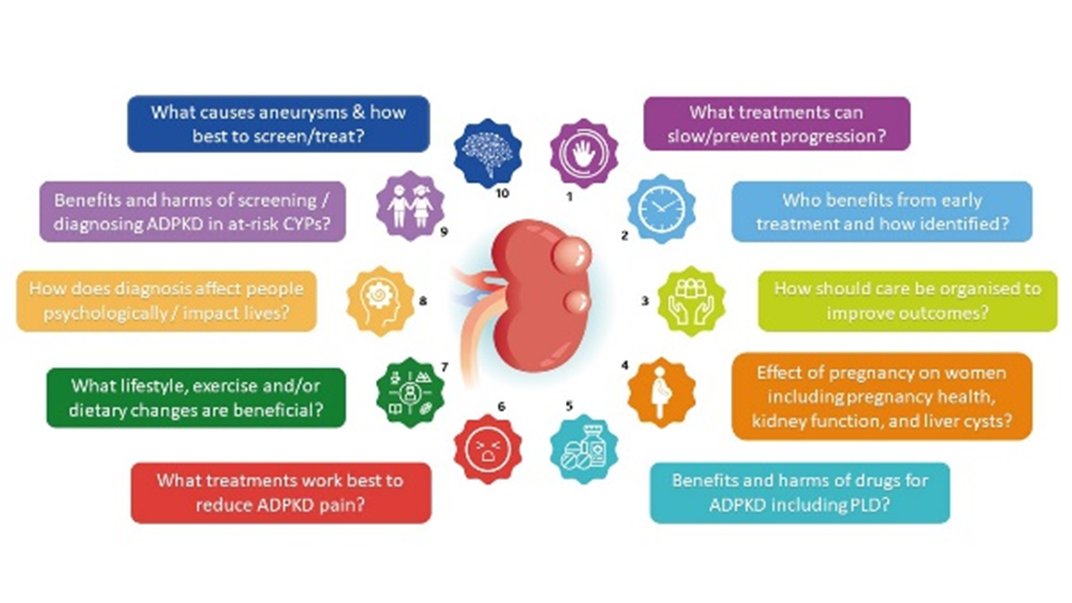
38) What do #ADPKD pts want researched? 🇬🇧Research Priority Setting Partnership Top 10: ⬇️progression, 🔎early progressors, care coordination, pregnancy🤰, #PLD, pain, lifestyle, #QOL, children, aneurysms 🔓
39) #ADPKD pts fortunate to have 🫶 pt/family communities/advocates w/wide & dedicated clinicians/research networks. #PKDOC @CPathInstitute @EuRefNetwork @song_initiative & all the PKD foundations, charities.
40) Thank you for your time! You just earned 0.5h CE/#CME credit and (hopefully) learned a lot about #ADPKD while doing it! So (a) go to https://ckd-ce.com/adpkd2/ to earn your credit & (b) FOLLOW @ckd_ce for more #tweetorial-based education about topics in #CKD mgt! I am @Elektra.
Originally tweeted by @CKD_ce (@ckd_ce) on April 19, 2022.